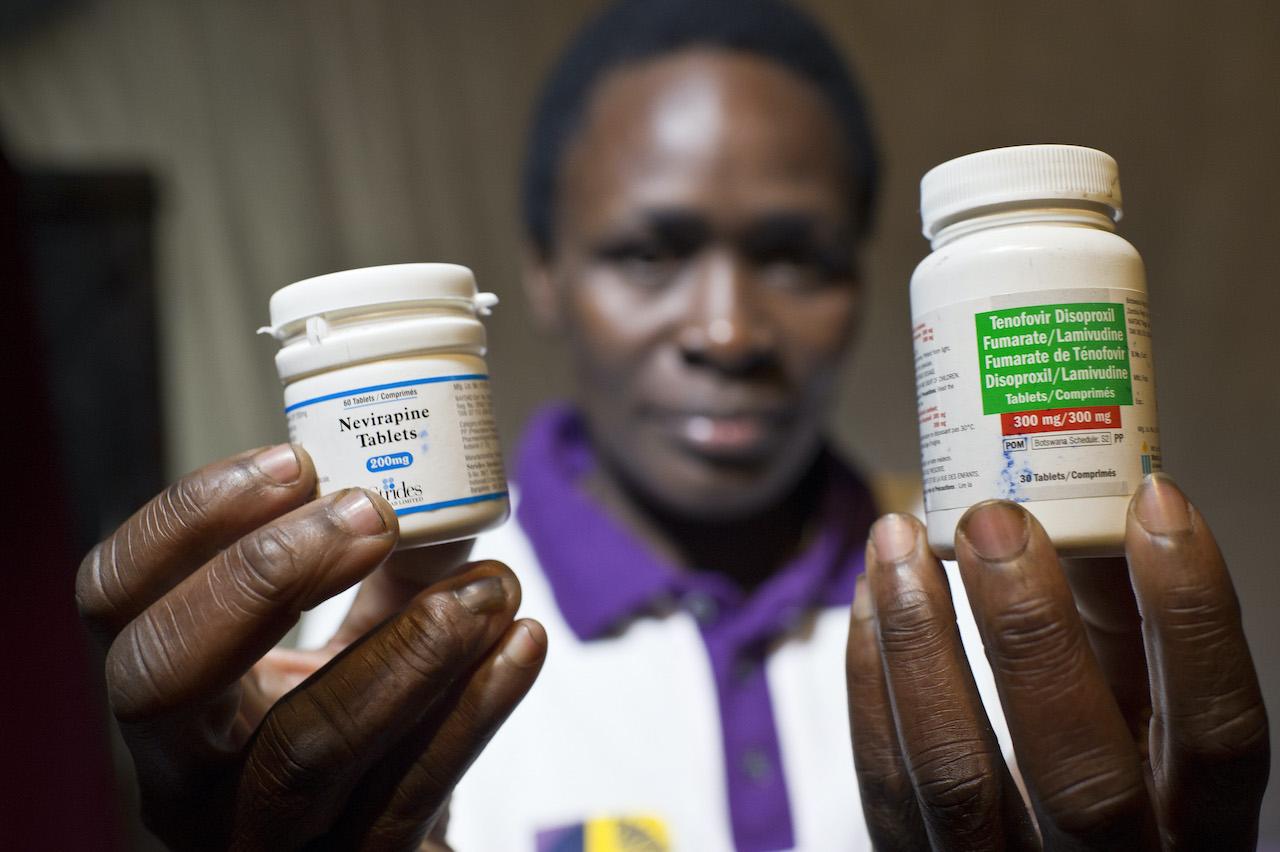
Homa Bay, Kenya -Unnecessary delays in releasing lifesaving HIV medicines to public health facilities is posing an imminent risk of stockouts, with devastating consequences for people living with HIV, warned the international medical organisation, Médecins Sans Frontières (MSF).
Essential HIV treatment drugs – Tenofovir, Lamivudine and Dolutegravir (TLD) – have been stuck at the port of Mombasa for several weeks and are not being distributed to the counties.
For the more than 114,000 people living with HIV (PLHIV) currently on treatment in Homa Bay County, 85% of whom are on TLD, impending stockouts risk forcing many to interrupt their treatment, wiping away recent gains in suppressing the deadly infection.
“Lack of timely access to HIV medications and the impending stockouts of ARVs is a tragedy waiting to happen and threatens to quash the gains made so far in reversing the curve of HIV infection in the county, which has the highest prevalence rates in the country – at 19.6% according to KENPHIA 2018 report,” says Roshni Mahida, the Project Coordinator for MSF in Homa Bay.
PLHIV are now forced to take between two- to four-week refilling schedules as limited supply of drugs threatens the long-term visibility and availability of the lifesaving medicines. Before the shortage, they would ordinarily be put on three- to six-month refills, and shorter treatment intervals were considered only for patients in need of closer follow up.
The long-term refills and medical review appointments are a cornerstone of the Differentiated Service Delivery (DSD) model – a patient-centred approach which simplifies and adapts HIV services to the needs of PLHIV while reducing unnecessary burdens on the health system – that has led to significant improvements in adherence to treatment in recent years.
Forty-year-old Milkah*, who has lived with HIV for close to 20 years, had to walk for close to five hours to the hospital because she could not raise the Kshs. 400 she needed for the fare to the facility to get her drug refills. “I left my house at 8:00 am and got to the hospital at 1:00 pm, only took 30 minutes at the hospital then began my journey back,” she says. “It’s a whole day affair and you get home very tired, yet you have kids to attend to.”
Indeed, this new schedule leads to additional costs of transport or more days off from work. Such disruptions in delivery schedules are additional stressors that can cause a variety of mental health issues.
When thirty-year-old Moses* went for his last clinical visit at Magina Health Centre in Ndhiwa Sub County mid-this month, he was given drugs to last him a month, down from the three. “We were told that there’s a shortage of drugs, the only problem is that I live far from here and the monthly visits will be difficult to arrange with my employer,” Moses says. He works and lives in Kisumu, which is some three-hour drive away, and expresses concern over the uncertainty over the future, should the drugs supply be disrupted. “Once you’ve accepted [to live with HIV] and started your treatment, a disruption of supply could be quite disheartening and could throw one into depression, considering the fatal consequences that may come with that supply cut,” he says.
For many years, HIV was the leading cause of morbidity and mortality in Homa Bay and in 2020 still, more than 37% of patients admitted into the county’s teaching and referral hospital adult internal medicine wards were HIV-positive.
“Against a backdrop of COVID-19 already disrupting the usual access and follow-up of PLHIV, we are likely to see a significant drop in adherence to treatment and viral load suppression, leading to a potential surge in infection rates unless an immediate solution to the impending ARV drugs stockout is found,” adds Roshni.