Doubting COVID-19, just narrowly surviving and facing stigma
KENNEDY MAGAK, 58, Boda boda (motoribike taxi) operator
“Three members of my family –my mother, my brother and I– got Covid... serious enough that we had to be admitted to the hospital. Unfortunately, my mother died, but my brother and I survived, just narrowly,” recalls Kennedy Magak.
For Kennedy, before he fell ill, his view on the coronavirus was similar to many other Homa Bay residents: ‘COVID-19 was just made up and a far-fetched rumour.’ So, he ignored the Ministry of Health’s (MoH) warnings and safety protocols and went about living a carefree life, oblivious of the fact that the virus was killing people in Homa Bay. Then Kennedy contracted the disease and spent one month in the hospital. Here he learnt the truth about this deadly virus. He spent four weeks in the High Dependency Unit, which changed his viewpoint forever. While fighting for his own life, he witnessed others also fighting for their lives. He will never doubt the virus again.
“I saw death hovering around my bed. People were dying around me and I thought the next minute it would be me. Unfortunately, when I left the hospital, it was my mother who was next. She died just because of our carelessness.”
Kennedy decided to become a patient activist because he knew people who still doubted the virus. Now he can share his painful story of personal loss and suffering. At his mother’s burial, he talked about his pain and what he saw at the hospital. He spread the word about the need to take precautions and told everyone about the seriousness of the disease. He talked about stigma because people were afraid to interact with him or anyone else who had been infected.
Kennedy has set up a hand washing point at the entrance to his home. He makes sure that everyone who visits is masked-up and they keep a safe, physical distance always.
Caring for family at bedside
ISAIAH WILLIS SUNDAYS, 67, Retiree
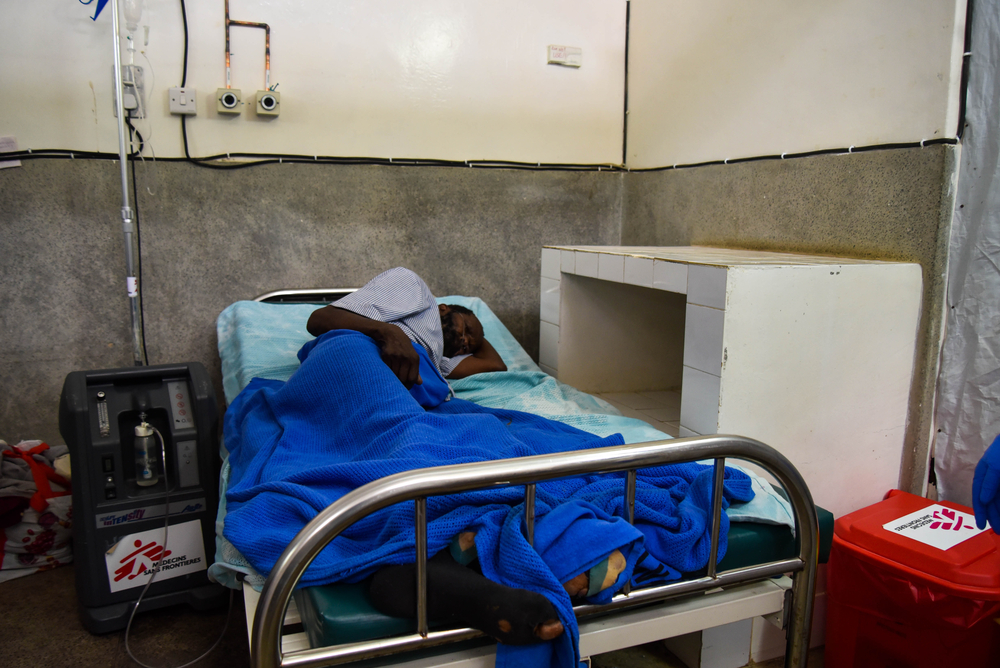
One week after Isaiah buried his wife, he started having difficulties breathing. Isaiah thought it was just his body responding to the exhausting ordeal of taking care of his sick wife and organizing the funeral.
Isaiah had started coughing even before his wife was buried. The cough then wasn’t so severe, so he just brushed it off as a normal thing but it worsened after the burial. He started feeling a lot of body pain and had a fever just like his wife, so he decided to go to the health center. They immediately referred him to the County Referral Hospital, where he tested positive for COVID-19. In fact, he was not just sick, but was critically ill so he was put in the High Dependency Unit and was hooked up to a high-flow oxygen unit.
“I remember that my wife was very tired and was coughing a lot. I took her to the local Gendia Hospital but was immediately referred to the hospital in Homa Bay. She tested positive for Covid and was admitted. She died four days later. My life is following the same sequence,” says Isaiah, with tears in his eyes as he recalled the memory.
The people in his village started avoiding him and his family after finding out that COVID-19 killed his wife, and that he also had the virus. His son, Francis, has refused to leave his bedside so he can monitor him –just as he behaved when his wife was sick.
"This is not something I’d wish for anyone"
JAMES OCHIENG ORONY, 45, School bursar

As a School Bursar, James has to interact with almost everyone who comes into the school building from teachers, students, staff, and visitors. He suspects this is how he contracted COVID-19.
“I must have caught the virus in school because the safety and prevention measures were not strict. Also, it seemed, everyone had lowered their guard, including me. As the Bursar, I had to meet many people who came to pay the school fees, so I was at high risk.
I feel that people at schools are not following the safety and prevention protocols. I see the hand washing points, but no one seems to be using them. Masks are often worn halfway or not worn at all. Staff are seeing these measures as a policy they can just ignore.
How I wish health promoters could visit schools to sensitize the teachers, staff, and students to understand the importance of safety and the risk of ignoring protocols while the virus is still spreading.
I had very painful headaches that I cannot even describe. I was admitted to the County Referral Hospital. I saw people cry. I saw them give up. I saw death moving from one bed to another. One minute you could be talking to someone, then the next minute you see his body being transferred to the morgue. In the evening, you sleep with two neighbours, but in the morning, they are gone.
This is not something I’d wish for anyone."
Due to the stigma surrounding COVID-19, he has met no one apart from his wife since being discharged.
MSF COVID-19 Response in Homa Bay
Since the start of the pandemic, MSF has had to progressively ramp up its support to the Homa Bay County Teaching and Referral Hospital by setting up additional beds in the COVID-19 High Dependency Unit (HDU) in tents inside the hospital compound to increase the bed capacity to 32 from the initial 10. During that period, MSF had a team of 60 staff to support a comprehensive programme of testing, case management, nutritional and psychosocial care, as well as assuring the supply of commodities, oxygen and electricity.
As cases and hospitalizations have declined since August, MSF has closed the extra beds in the HDU and continues to support COVID-19 patients with regular follow-up after their discharge, provide daily supervision of the remaining patients, and continue testing of suspect patients in the Outpatient Department triage and adult internal medicine wards.
