
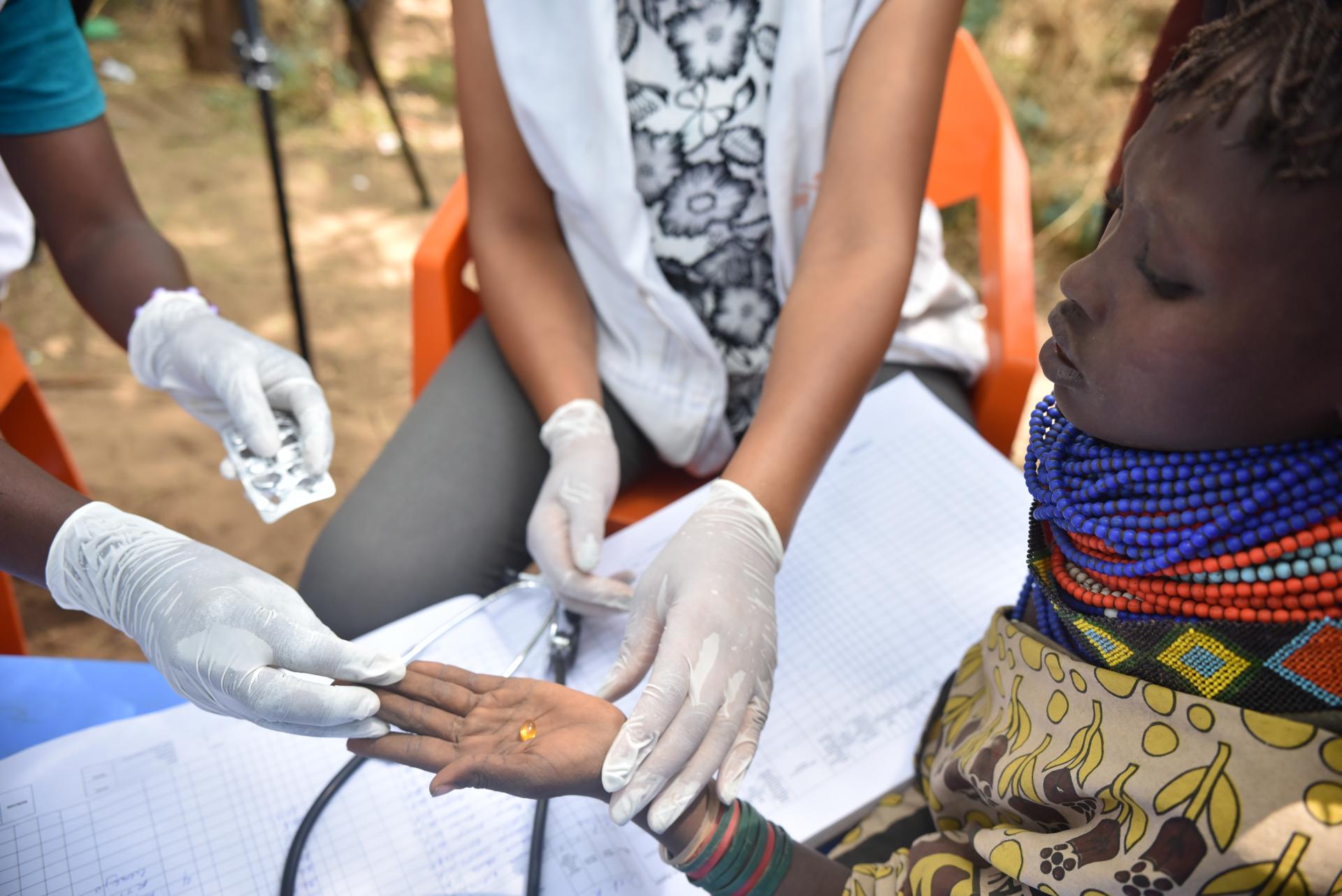
Kenya
Drought and conflict in Somalia continued to drive people to seek refuge in Dadaab, a huge, overcrowded camp complex in Kenya, which currently hosts more than 350,000 registered and unregistered refugees. Our teams delivered healthcare in and around the complex, in particular in Dagahaley camp, while publicly and persistently calling for an improved international response to scale up humanitarian assistance.

3,840
3,84
3,490
3,49
11,500
11,5
10,700
10,7
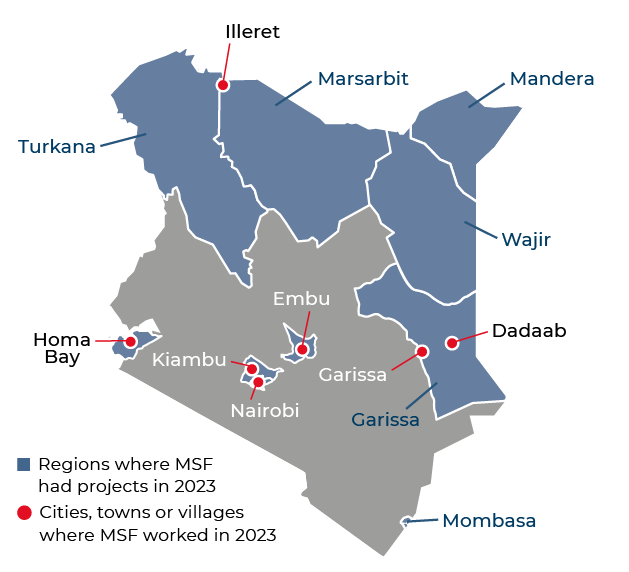
Our activities in 2023
We provided social and medical assistance to marginalised communities in Mombasa and Nairobi, and in Kiambu county.
In Mombasa, we supported numerous facilities to cater to the specific needs of vulnerable adolescents and young people, including people who engage in sex work, people who use drugs intravenously, people from the LGBTQI+ community, and individuals living on the streets.
In Nairobi’s Eastlands suburb, the youth-friendly centre we run in a public facility continued to assist people affected by violence by offering medical services, including sexual and reproductive healthcare, as well as psychosocial support, recreational activities and educational programmes. gunshot wounds, as well as orthopaedic trauma, burns and other conflict-related injuries. Our holistic approach to care includes physiotherapy and mental health support. In 2023, we continued to develop our regional outreach to facilitate follow-up consultations and continued physiotherapy for patients in their home countries, after discharge from the hospital. MSF collaborates closely with local healthcare providers, offering technical assistance, training and medical supplies to bolster healthcare capacity.
In Kiambu county, we worked with the local government to implement effective healthcare solutions for people who use drugs, such as offering medically assisted therapy in smaller, local clinics close to where they live.
Our teams also responded to several emergencies in 2023. In November, the northeast of Kenya experienced significant rainfall, resulting in flooding that displaced thousands of families. We launched a rapid emergency response to deliver medical care and distribute hygiene kits to affected communities.
In Ileret, Marsabit county, we drilled wells to provide access to clean water, and treated malnutrition. In Mandera, we responded to a cholera outbreak with treatment for patients and community outreach activities, while in Turkana, our teams conducted vaccinations and offered treatment for malnutrition, malaria and measles.
Throughout the year, we continued to work on improving HIV care in the country. In Homa Bay, we supported the county referral hospital’s adult medical wards with staff, treatment and follow-up care.
1987
1987
755
755
€23 M
23M


Can you share an inspiring story of a woman who has made a positive impact in your community or organisation?

Breaking down stigmas and barriers to care in Mombasa, Kenya

Dadaab, Kenya: MSF completes Mass Drug Campaign to tackle Schistosomiasis in Dagahaley Refugee Camp

MSF climate change workshop looks ahead to grim regional health outlook
