Dr. Sanne Burkert, HIV Doctor in Homa Bay
“ My name is Sanne Burkert and I am a medical doctor from Germany in a first time assignment with MSF. After my graduation from medical school, I worked in a German hospital, obviously a contrast from Homa Bay context as it is a high resource setting. MSF is one organisation that you will hear about constantly together with ICRC. During my studies, I attended MSF talks in Berlin, and knew that one day I would be good enough to be part of the MSF projects. I always thought that I should be fully specialized to work with MSF, which I still am not, but felt at some point that I am probably skilled enough and applied. Sometimes we think that we have to be very experienced or specialise for many years and thus it becomes difficult to find the right time to apply.
Homa Bay project is one of the long-standing projects in Kenya and has the highest HIV prevalence(Kenya Population-based HIV Impact Assessment (KENPHIA) 2018 survey) in the country. Mortality rate was so high before the introduction of Antiretroviral drugs, and right now, the project also focuses on non-communicable diseases(NCDs), chronic diseases, supporting the inpatient wards, HIV patients, and all adult medical patients.
It was fairly easy for me to become a doctor, as well as getting medical access, but growing up, I knew that that was not the ideal world for everyone. So, I thought of contributing in making it a more equal world thus the humanitarian thought of working in places where people do not have it easier, that is, becoming a doctor easily or accessing a doctor because the doctor patient ratio is quite low.
I get to work at 8 am for a hand over from the night doctor, the next one hour is to organise myself. From 9am, I start the ward rounds and sometimes we do it with the consultant. This takes two to four hours depending on the patients I have and the conditions being treated. I then follow this up with some meetings if need be, while also doing diagnostic and therapeutic procedures at the hospital. I take a lunch break at 1PM and in between check on the patients. I handover to the next doctor at 5pm, and may extend at times depending on what needs to be done.
The HIV/AIDS epidemic is still an ongoing fight even with reduced mortality, and it is quite clear that if MSF would not be here, there would be more deaths witnessed as a result of HIV infections. MSF has also enabled care to be accessible at the Homa Bay County Teaching and Referral Hospital and through the decentralized sites where we provide chronic disease care, ensuring health services are accessible at the community level. The advanced HIV patients are mostly younger, and, unfortunately, still present in an advanced AIDS stage with many infections.
We are one of the few projects in MSF that have indirect access to dialysis, but still it gives us and the patients a lot of trouble. The referral hospital is the main public facility in Homa Bay where patients receive dialysis, but many times, the dialysis is not working and in cases of kidney failure, it can be catastrophic. The process of getting a dialysis by these patients is hectic. They need a lot of money if they don’t have an insurance cover and most times they cannot afford either, and have to seek support from the hospital for waivers. With kidney failure, time is a factor. We lose patients sometimes because of the steps it takes.
There was this lady that came with kidney failure very late and the dialysis department was not working well. The next day on Monday, we put a lot of effort into hastening the hospital processes to ensure that by afternoon the dialysis was ready. I finally put the dialysis catheter in the evening hours and she started to get better for the next few days. My next ward round on Thursday, she waved at me and called out telling me she was thankful that I had saved her life with her whole family there. That felt very good! One patient appreciating what we do makes a huge difference and that doesn’t happen always. And it was good for the whole team to see that with effort, patients can get better, because at some point we all thought she would not make it.
My main challenge is accepting that for some patients, you cannot do anything and not take it as a personal failure. In an ideal setting, you could do more, but here due to limited resources, you cannot do as much as you would wish. In such instances, beyond acceptance, it is also a chance for you to address challenges by starting a process to get solutions. And that’s mostly why MSF is here.
As a doctor, you are at the ward every time and you have a choice to either repeat instructions every time patients need treatment, or create a structure to address them. This is what has led me to create a simplified standard operating procedure (SOP) for acute kidney failure addressing some gaps that were in the initial assessment guideline. Also created a checklist for anaemia investigation to ensure proper assessment of patients, with the tool now adopted by the team and revised an antibiotics standard operating procedures (SOP) on rational prescription based.
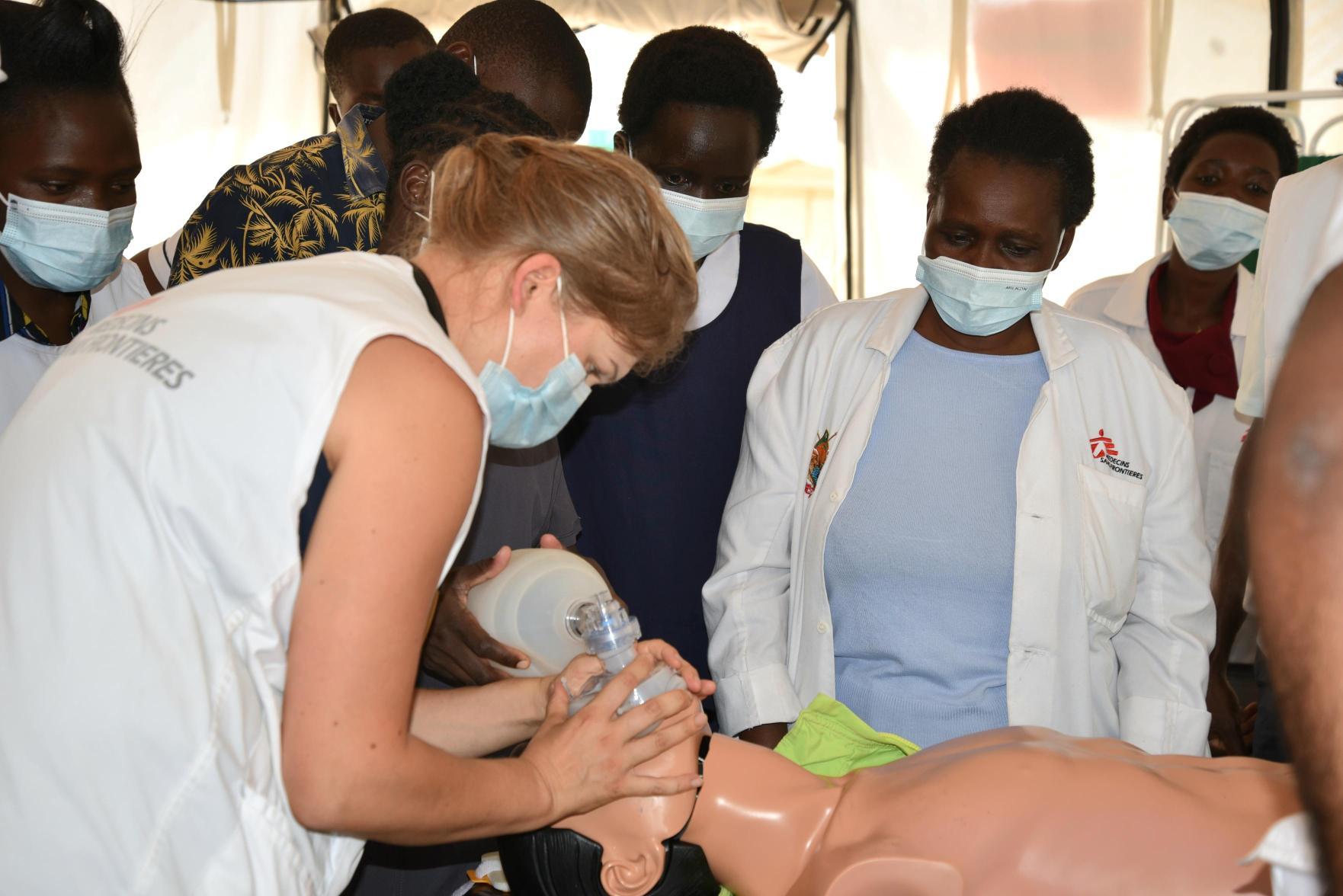
We recently did CPR training for resuscitation as we had noted some instances when it was not working well in the wards. I figured out that staff needed more training. And based on experience, I knew the type of training the team needed.
The Homa Bay project is a safe environment but very challenging. You cannot achieve everything that you want to do for every patient mainly because of the insufficient commodities, limited financial and personnel resources. This may lead to frustrations and lack of motivation. However, you need to realise that you yourself can make a difference!
Being a doctor, you interact with so many people, and patients, from different levels in the society, and the poorest of the societies. You have a good access to a world you are normally not a part of, and with different professionals too. It is exciting that I now know more than the sixty staff at the hospital. In the beginning, I could not distinguish people especially with them wearing masks in the first month. I had to ask their names several times and reintroduce myself.
The best memory for me is the swimming classes we do for the team on Sundays, in the only swimming pool in Homa Bay.
As my mission ends, I will take time to reflect and prepare for the next mission once ready!”